Abstract
Purpose
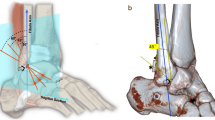
A bone tunnel is often used during the reconstruction of the anterior talofibular ligament (ATFL) and calcaneofibular ligament (CFL). The purpose of this study is to compare proposed directions for drilling this fibular tunnel and to assess potential tunnel length, using a 5-mm-diameter tunnel and surrounding bone.
Methods
Anonymous DICOM data from spiral CT-scan images of the ankle were obtained from 12 Caucasian patients: 6 females and 6 males. Virtual tunnels were generated in a 3D bone model with angles of 30°, 45°, 60° and 90° in relation to the fibular long axis. Several measurements were performed: distance from entrance to perforation of opposing cortex, shortening of the tunnel, distance from tunnel centre to bone surface.
Results
A tunnel in a perpendicular direction resulted in an average possible tunnel length of 16.8 (± 2.7) mm in the female group and 20.3 (± 3.4) mm in the male group. A tunnel directed at 30° offered the longest length: 30.9 (± 2.5) mm in the female group and 34.4 (± 2.9) mm in the male group. The use of a 5-mm-diameter tunnel in a perpendicular direction caused important shortening of the tunnel at the entrance in some cases. The perpendicular tunnel was very near to the digital fossa while the most obliquely directed tunnels avoided this region.
Conclusion
An oblique tunnel allows for a longer tunnel and avoids the region of the digital fossa, thereby retaining more surrounding bone. In addition, absolute values of tunnel length are given, which can be useful when considering the use of certain implants. We recommend drilling an oblique fibular tunnel when reconstructing the ATFL and CFL.




Similar content being viewed by others
References
Caprio A, Oliva F, Treia F, Maffulli N (2006) Reconstruction of the lateral ankle ligaments with allograft in patients with chronic ankle instability. Foot Ankle Clin 11:597–605
Clanton TO, Campbell KJ, Wilson KJ, Michalski MP, Goldsmith MT, Wijdicks CA, LaPrade RF (2014) Qualitative and quantitative anatomic investigation of the lateral ankle ligaments for surgical reconstruction procedures. J Bone Joint Surg Am 96:e98. https://doi.org/10.2106/JBJS.M.00798
Clanton TO, Viens NA, Campbell KJ, Laprade RF, Wijdicks CA (2014) Anterior talofibular ligament ruptures, part 2: biomechanical comparison of anterior talofibular ligament reconstruction using semitendinosus allografts with the intact ligament. Am J Sports Med 42:412–416
Golano P, Vega J, de Leeuw P, Malagelada F, Manzanares MC, Götzens V, van Dijk CN (2010) Anatomy of the ankle ligaments: a pictorial essay. Knee Surg Sports Traumatol Arthrosc 18:557–569
Guillo S, Archbold P, Perera A, Bauer T, Sonnery-Cottet B (2014) Arthroscopic anatomic reconstruction of the lateral ligaments of the ankle with gracilis autograft. Arthrosc Tech 22(3):e593–e598
Guillo S, Bauer T, Lee JW, Takao M, Kong SW, Stone JW, Mangone PG, Molloy A, Perera A, Pearce CJ, Michels F, Tourné Y, Ghorbani A, Calder J (2013) Consensus in chronic ankle instability: aetiology, assessment, surgical indications and place for arthroscopy. Orthop Traumatol Surg Res 99:411–419
Guillo S, Cordier G, Sonnery-Cottet B, Bauer T (2014) Anatomical reconstruction of the anterior talofibular and calcaneofibular ligaments with an all-arthroscopic surgical technique. Orthop Traumatol Surg Res 100:S413–S417
Higashiyama R, Aikawa J, Iwase D, Takamori Y, Watanabe E, Takaso M (2019) Anatomical arthroscopic anterior talofibular ligament and calcaneofibular ligament reconstruction using an autogenic hamstring tendon: safe creation of anatomical fibular tunnel. Arthrosc Tech 8(3):e215–e222
Jeys L, Korrosis S, Stewart T, Harris NJ (2004) Bone anchors or interference screws? A biomechanical evaluation for autograft ankle stabilization. Am J Sports Med 32(7):1651–1659
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15:155–163
Krähenbühl N, Weinberg MW, Davidson NP, Mills MK, Hintermann B, Saltzman CL, Barg A (2018) Currently used imaging options cannot accurately predict subtalar joint instability. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-018-5232-8
Kuo CC, Lu HL, Leardini A, Lu TW, Kuo MY, Hsu HC (2014) Three-dimensional computer graphics-based ankle morphometry with computerized tomography for total ankle replacement design and positioning. Clin Anat 27:659–668
Li H, Hua Y, Li H, Chen S (2018) Anatomical reconstruction produced similarly favorable outcomes as repair procedures for the treatment of chronic lateral ankle instability at long-term follow-up. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-5176-z
Matsui K, Oliva XM, Takao M, Pereira BS, Gomes TM, Lozano JM, ESSKA AFAS Ankle Instability Group, Glazebrook M (2017) Bony landmarks available for minimally invasive lateral ankle stabilization surgery: a cadaveric anatomical study. Knee Surg Sports Traumatol Arthrosc 25(6):1916–1924
Matsui K, Takao M, Tochigi Y, Ozeki S, Glazebrook M (2017) Anatomy of anterior talofibular ligament and calcaneofibular ligament for minimally invasive surgery: a systematic review. Knee Surg Sports Traumatol Arthrosc 25(6):1892–1902
Michels F, Clockaerts S, Van Der Bauwhede J, Stockmans F, Matricali G (2019) Does subtalar instability really exist? A systematic review. Foot Ankle Surg. https://doi.org/10.1016/j.fas.2019.02.001
Michels F, Cordier G, Burssens A, Vereecke E, Guillo S (2016) Endoscopic reconstruction of CFL and the ATFL with a gracilis graft: a cadaveric study. Knee Surg Sports Traumatol Arthrosc 24(4):1007–1014
Michels F, Cordier G, Guillo S, Stockmans F, ESKKA-AFAS Ankle Instability Group (2016) endoscopic ankle lateral ligament graft anatomic reconstruction. Foot Ankle Clin 21:665–680
Michels F, Guillo S, Vanrietvelde F, Brugman E, Ankle Instability Group, Stockmans F (2016) How to drill the talar tunnel in ATFL reconstruction? Knee Surg Sports Traumatol Arthrosc 24(4):991–997
Michels F, Pereira H, Calder J, Matricali G, Glazebrook M, Guillo S, Karlsson J, ESSKA-AFAS Ankle Instability Group (2018) Searching for consensus in the approach to patients with chronic lateral ankle instability: ask the expert. Knee Surg Sports Traumatol Arthrosc 26:2095–2102
Neuschwander T, Indressano A, Hughes T, Smith B (2013) Footprint of the lateral ligament complex of the ankle. Foot Ankle Int 34:582–586
Takao M, Oae K, Uchio Y, Ochi M, Yamamoto H (2005) Anatomical reconstruction of the lateral ligaments of the ankle with a gracilis autograft: a new technique using an interference fit anchoring system. Am J Sports Med 33:814–823
Vuurberg G, Pereira H, Blankevoort L, van Dijk CN (2018) Anatomic stabilization techniques provide superior results in terms of functional outcome in patients suffering from chronic ankle instability compared to non-anatomic techniques. Knee Surg Sports Traumatol Arthrosc 26(7):2183–2195
Wang B, Xu XY (2013) Minimally invasive reconstruction of lateral ligaments of the ankle using semitendinosus autograft. Foot Ankle Int 34:711–715
Weiler A, Hoffmann RF, Siepe CJ, Kolbeck SF, Südkamp NP (2000) The influence of screw geometry on hamstring tendon interference fit fixation. Am J Sports Med 28(3):356–359
Youn H, Kim YS, Lee J, Choi WJ, Lee JW (2012) Percutaneous lateral ligament reconstruction with allograft for chronic lateral ankle instability. Foot Ankle Int 33:99–104
Funding
No funding was received by any of the authors related to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The present study was approved by the Ethics Committee of X (BUN B396201835645).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Michels, F., Matricali, G., Guillo, S. et al. An oblique fibular tunnel is recommended when reconstructing the ATFL and CFL. Knee Surg Sports Traumatol Arthrosc 28, 124–131 (2020). https://doi.org/10.1007/s00167-019-05583-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-019-05583-3